
Understanding your lab values is essential to managing your kidney disease. These values are monitored regularly and play a critical role in helping you and your healthcare provider:
- Track how well your kidneys are functioning
- Detect complications early
- Manage symptoms more effectively
- Guide treatment decisions to slow the progression of kidney disease
By learning what each lab value means, you can take a more active role in your care. This knowledge empowers you to ask informed questions, engage in meaningful conversations with your healthcare team, and ensure your questions and/or concerns are fully addressed. This brochure defines many of the tests and lab values that are important in managing kidney disease.
Kidney Function
Kidneys play a very important role in keeping your entire body functioning properly and have many responsibilities. One of those is to help filter waste and toxins from your blood and remove extra fluid from your body. Filtering waste from the blood is essential for survival and protects every system in the body.
Creatinine, eGFR, uACR, and BUN are crucial markers for kidney patients. Your doctor will look at these to help determine how well your kidneys are working and removing waste.
Creatinine
Creatinine is a waste product made by your muscles from the breakdown of a compound called creatine. Because the kidneys are responsible for removing creatinine from your body, monitoring the amount of creatinine in your blood is a key way to check on the health of your kidneys.
There are several reasons why a creatinine level may be high – it could be a sign of worsening kidney function but it could also indicate dehydration, certain medications, infections, or possibly a diet very high in protein.
Your creatinine is used to calculate your estimated Glomerular Filtration Rate (eGFR), another key marker of your kidney’s function.
Estimated Glomerular Filtration Rate (eGFR)
One of the key markers for kidney function is your estimated Glomerular Filtration Rate (eGFR). It estimates how well your kidneys are filtering waste, toxins, and extra fluid from your body every minute. The eGFR is also useful to help detect kidney disease, track progression of the kidney disease, and also help guide treatment decisions.
The eGFR calculation is based on your blood creatinine level, age, sex, and sometimes race. It calculates how much blood is passing through the glomeruli (tiny filtering units in your kidneys) each minute.
The eGFR level is used to help determine how severe your kidney damage is from Stage 1 (mild) chronic kidney disease (CKD) to Stage 5 (end stage kidney failure).
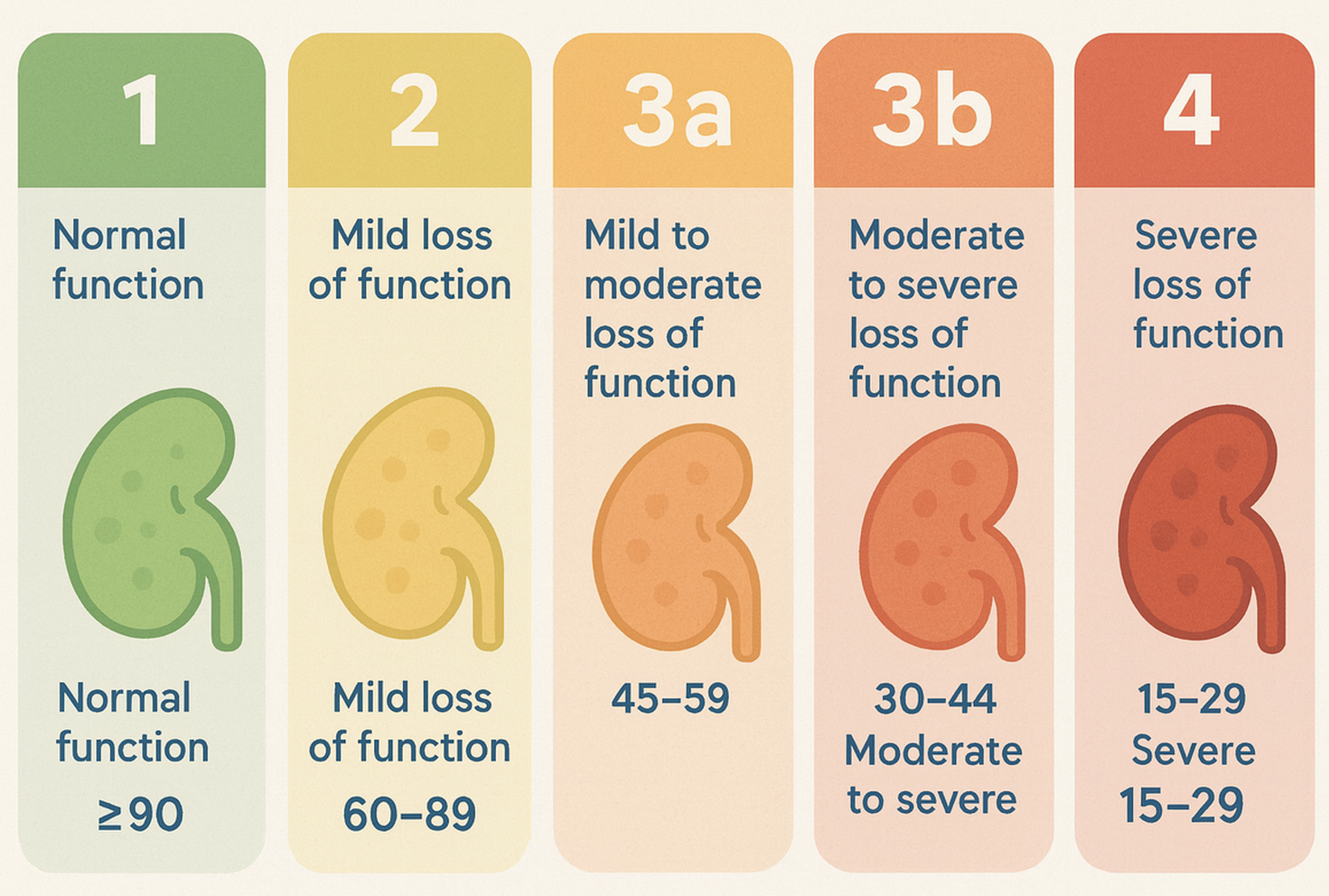
Because your eGFR may fluctuate slightly based on your hydration status, medications you are taking (including over-the-counter medications), illness, and even your muscle mass, your healthcare provider will use the eGFR to help decide whether to start or stop medication. It is also used to help decide when you get referred to a nephrologist, and when to help prepare for dialysis or transplantation.
Urine Albumin-to-Creatinine Ratio (uACR)
The Urine Albumin-to-Creatinine Ratio (uACR) test is a tool to check for kidney damage. If you have diabetes or high blood pressure, you should have a uACR test regularly.
The presence of albumin (a protein found in the blood) in the urine (called albuminuria or proteinuria) is one of the earliest signs your kidneys are leaking protein, which is a sign of kidney disease.
The uACR test counts the amount of albumin in your urine compared to creatinine (a waste product, mentioned above). The result of your uACR is used together with your eGFR to determine the stage of kidney disease and the risk of your kidney disease progressing.
A high uACR is often linked with a higher risk of kidney failure, heart disease, and death.
Considerations if your uACR is elevated:
- Control blood sugar
- Manage blood pressure
- Reduce salt and protein intake
- Your healthcare provider may suggest taking kidney-protective medications like:
- » ACE inhibitors (a type of medication that » ARBs (another type of medication that lowers blood pressure), or
- » SGLT2 inhibitors (a type of medication used to treat type 2 diabetes)
Blood Urea Nitrogen (BUN)
The Blood Urea Nitrogen (BUN) is a common blood test that measures how much urea nitrogen is in your blood. When your body breaks down protein from food, it creates urea. Urea is a waste product. Urea travels through your blood to your kidneys and the kidneys will normally filter it out into your urine.
If you have kidney disease, urea builds up in your blood and causes a high BUN level. That is why the BUN value is another key marker when you have kidney disease as it helps assess how well your kidneys are removing waste products from your body.
BUN may also rise in the setting of dehydration, bleeding, high protein intake, or heart failure.
Along with your creatinine and your eGFR, your BUN is used to evaluate and track your CKD.
Electrolytes
Healthy kidneys are necessary for managing electrolytes. Electrolytes are minerals with an electric charge that are essential for bodily functions like nerve and muscle function, hydration, and maintaining pH balance. While the kidneys are filtering waste from your blood, they are also deciding how much of each electrolyte stays in the body and how much is removed from the body through the urine. Electrolytes that are important for kidney health include: potassium, sodium, calcium, phosphorus, and bicarbonate.
Potassium (K)
Potassium (K) is a mineral and electrolyte that is very important in regulating your heart rhythm and in supporting muscle and nerve function.
Your kidneys are responsible for filtering out excess potassium from your blood through the urine. If your kidneys cannot filter potassium, potassium will build up in the bloodstream. A high potassium level, also known as hyperkalemia, is life threatening because it may cause cardiac arrest. Learn more about potassium at www.areyouok.org and mark your calendar for National High Potassium Awareness Day (May 1st).
Sodium (Na)
Sodium (Na) is an electrolyte and is a mineral closely monitored to assess your fluid and blood pressure. When you have kidney disease, your kidneys may not be able to get rid of excess sodium. Excess sodium, also called hypernatremia, may lead to fluid retention, swelling (edema), high blood pressure (hypertension), and even congestive heart failure.
Calcium (Ca)
Calcium (Ca) is an electrolyte and a is a very important mineral in keeping bones and teeth strong and healthy. Calcium balance can be disrupted in kidney disease leading to serious complications which is why your calcium must be monitored closely in kidney disease. A high level of calcium in the blood is called hypercalcemia which can lead to various symptoms and complications such as bone weakening, kidney stones, and heart and brain dysfunction.
Calcium is the main mineral in bones (about 99% of calcium is stored there). Maintaining a balanced level of calcium in the blood is very important as it keeps our bones and teeth healthy but also helps with nerve function, muscle contractions, and blood clotting.
Calcium is closely regulated by other minerals and hormones, such as the parathyroid hormone, vitamin D, and calcitonin, a hormone produced by the thyroid gland that helps to lower blood calcium levels.
Hyperkalemia:
high potassium level in blood
Hypernatremia:
high sodium level in blood
Hypercalcemia:
high calcium level in blood
Bone and Mineral Balance
Kidneys play a key role in regulating calcium (see above) and other minerals, such as phosphorus, in your body.
Ensuring your bone-mineral levels are well-managed will aid in reducing long-term complications such as weak bones, calcium deposits in blood vessels, and heart disease.
Phosphorus (P)
Phosphorus (P) is another important electrolyte and mineral that is essential for bone formation, energy metabolism, and cell function. About 85% of phosphorus is stored in bones.
The kidneys are primarily responsible for helping maintain a balanced level by removing excess phosphorus. When the kidneys are not properly functioning, phosphorus can build up, causing hyperphosphatemia, and can bind with calcium pulling calcium out
of the bone - this causes those
calcium deposits (vascular calcification) and weak bones.
Learn more about phosphorus at
www.thehiddenpinkidneydisease.org and mark your calendar for National Phosphorus Awareness Day (April 5th).
Vitamin D
Vitamin D is a fat-soluble vitamin essential for bone health, immune function, and maintaining a balance between your calcium and phosphorus levels.
Vitamin D is inactive when first consumed and healthy kidneys activate that inactive vitamin D to an active form called calcitriol. This activation is a necessary step in helping your body absorb calcium from food.
When kidneys are not functioning properly, they cannot convert vitamin D into calcitriol so less calcium is absorbed from the intestines. Reduced calcium absorption may lead to low levels of calcium.
Because vitamin D is needed for calcium absorption, if the kidneys are not fully working, vitamin D will remain inactive, leading to: 1) low calcium 2) bone loss 3) overactive parathyroid glands (known as secondary hyperparathyroidism), and 4) higher risk of fractures.
Parathyroid Hormone (PTH)
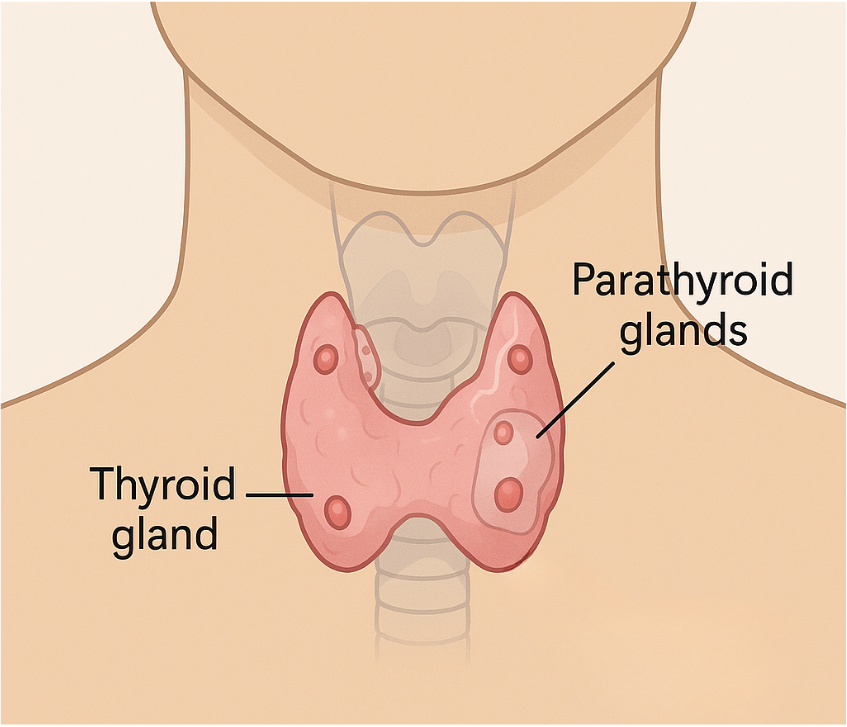
The parathyroid glands are small endocrine glands (specialized organs that produce and secrete hormones) located behind your thyroid gland. The main function of the parathyroid glands is to regulate the level of calcium in your blood by producing a hormone called parathyroid hormone (PTH).
If the calcium level drops in your blood, the parathyroid glands will release PTH.
PTH works to increase calcium in the blood by:
- Releasing calcium from bones
- Increasing kidney reabsorption of calcium
- Activating vitamin D by increasing intestinal calcium absorption
- Promoting phosphate excretion
High levels of PTH is common in CKD. When PTH is high, it will pull calcium from bones and can cause bones to release calcium into the blood. Over time, this will weaken bones.
Secondary hyperparathyroidism is a condition in which the parathyroid glands produce too much PTH because of chronic low calcium levels caused by CKD. The effects of high PTH and low calcium include: renal osteodystrophy (a bone disease that occurs when CKD causes imbalances in minerals and hormones needed for healthy bones), calcification of blood vessels and tissues, muscle weakness, and joint pain. In some cases, a parathyroidectomy, or surgical removal of one or more parathyroid glands, may be considered to reduce these risks.
Hyperphosphatemia:
a condition when the phosphorus in the blood becomes higher than it should be
Hyperparathyroidism:
a condition where your body produces too much parathyroid hormone which can cause problems with your blood, bones, and kidneys
Renal osteodystrophy:
a bone disease that occurs when CKD causes imbalances in minerals and hormones needed for healthy bones
Parathyroidectomy:
surgical removal of one or more parathyroid glands
Anemia
Red blood cells (RBC) are the cells that travel throughout your body delivering oxygen to your organs, muscles and tissues. Anemia is when you do not have enough healthy red blood cells or hemoglobin to carry oxygen throughout the body. The kidneys are important in preventing anemia because they control the production of RBCs by making a very important hormone called erythropoietin.
Erythropoietin (EPO)
Erythropoietin (EPO) is a hormone produced by the kidneys and is released when the kidneys sense low oxygen levels in your blood. The hormone will tell your bone marrow to make red blood cells. When the kidneys are damaged, they may not produce enough EPO, so fewer RBCs are made, resulting in anemia.
Treatment for anemia associated with kidney disease typically includes:
- Iron supplements (oral or intravenous)
- Erythropoiesis-stimulating agents (ESA) which are injected under the skin (subcutaneously)
- Treating underlying causes like low vitamin B12 or chronic blood loss
Hemoglobin (Hb)
Hemoglobin (Hb) is a protein in red blood cells (RBCs) that transports oxygen from your lungs to the rest of your body. If you do not have enough hemoglobin, your organs, muscles and tissues will not get enough oxygen, leading to anemia.
If the hemoglobin drops too low, you may be at risk of heart failure because severe anemia makes your heart work harder.
Symptoms of anemia in CKD include:
- Fatigue
- Shortness of breath
- Weakness
- Pale skin
- Difficulty concentrating
- Reduced ability to exercise
- Chest pain or heart palpitations in severe anemia
Iron Studies (Ferritin, Transferrin Saturation)
Testing for iron helps your healthcare provider manage your anemia and provides them with a guide on what type of iron therapy may be needed. Iron is needed to create hemoglobin, the protein in red blood cells that carries oxygen from the lungs to the rest of the body.
Your healthcare provider may also screen your B12 and folate (vitamin B9) levels, as low levels of these may also lower hemoglobin.
Diabetes Screening
Screening for diabetes is very important because high blood sugar can damage the small blood vessels in the kidneys. Over time, this damage can lead to chronic kidney disease or even kidney failure.
Hemoglobin A1C (HbA1c)
Hemoglobin A1C (HbA1c) measures your average blood sugar level over the past 2-3 months and reflects how much glucose (sugar) has been attached to your red blood cells.
Hb A1c is an important tool to screen for diabetes. For persons with diabetes, it is also an important marker to evaluate how well the diabetes is being managed. Because diabetes is the leading cause of CKD, the HbA1c is especially important since uncontrolled blood sugar control contributes to worsening kidney disease by damaging the blood vessels in the kidneys. Over time this leads to protein in the urine, progression of the kidney disease, and even kidney failure.
The ideal HbA1c goal will depend on your stage of CKD, age and other health issues. Ensuring your Hgb A1c stays in a safe range will lower your risk of heart disease, nerve damage, and vision loss.
It is important to know that in later stages of CKD, HbA1c may be less reliable due to anemia, short red blood cell lifespan, or use of erythropoiesis-stimulating agents (ESA medications). In that case, your healthcare provider may also include a continuous glucose monitoring (CGM) device to assist with monitoring your blood sugar.
Urine Tests
Urine tests are an important tool when screening for kidney disease. Often, urine tests may show early signs of kidney disease – even before blood tests or before someone may have any physical symptoms of kidney disease.
Urinalysis
A urinalysis screens for protein in the urine (proteinuria), blood in the urine (hematuria), and other abnormalities, such as glucose (sugar) in the urine.
This test will also screen for white blood cells and nitrites – two signs that can indicate a urinary tract infection (UTI), which can worsen your kidney function if left untreated.
Albumin
Albumin is a protein made by the liver and works to keep fluid in your blood. If your body does not have enough albumin, fluid will leak into the tissues and cause swelling. Healthy kidneys help keep albumin in your blood where it belongs.
When kidneys are not properly functioning, albumin can leak into the urine, which is called albuminuria. High levels of albumin in urine is an early sign of kidney damage, which often appear before other symptoms. Low levels of albumin may suggest you are losing protein in your urine and may also indicate malnutrition.
The albumin level provides key information about your kidney function, nutritional status, and overall health and will be monitored to help track the progression of CKD.
Fluid and Acid-Base Balance
Kidneys are constantly monitoring and adjusting the amount of water and chemicals in your blood and tissues. Healthy kidneys are necessary to keep your body’s internal environment healthy and well-balanced.
Bicarbonate (HCO3-)
Bicarbonate (HCO3-) is an electrolyte and an alkaline substance (a substance that dissolves in water) that helps counteract excess acid in your blood. Healthy kidneys reabsorb bicarbonate and help to keep your blood pH (measure of the acidity or alkalinity of blood) stable.
In CKD, kidneys are not able to perform this function, leading to metabolic acidosis, or too much acid in the blood. Metabolic acidosis can worsen kidney damage.
Your bicarbonate level helps determine whether you will need to take oral sodium bicarbonate tablets or adjust your diet to help neutralize your blood.
Understand Your Lab Values!
Routine lab work is essential to managing your kidney disease and protecting your overall health. By learning and understanding your lab values, you will be an active participant in protecting your kidneys. As you keep track of lab values on your own, you can compare results from one report to another. Are they consistent? Is something higher or lower than previous labs? You can ask your doctor to explain any changes.
Benefits of understanding your lab values:
- Detect problems early
- Slow the progression of your kidney disease
- Avoid serious complications
- Improve quality of life and survival
- Know which lab values to ask your healthcare team about
- Participate in informed discussions with your healthcare team about what you can do to manage levels
Below is an example of a lab report you may have seen before, along with guidance on how to read and understand it.
Understanding your lab values is essential to managing your kidney disease. These values are monitored regularly and play a critical role in helping you and your healthcare provider:
- Track how well your kidneys are functioning
- Detect complications early
- Manage symptoms more effectively
- Guide treatment decisions to slow the progression of kidney disease
By learning what each lab value means, you can take a more active role in your care. This knowledge empowers you to ask informed questions, engage in meaningful conversations with your healthcare team, and ensure your questions and/or concerns are fully addressed. This brochure defines many of the tests and lab values that are important in managing kidney disease.
Kidney Function
Kidneys play a very important role in keeping your entire body functioning properly and have many responsibilities. One of those is to help filter waste and toxins from your blood and remove extra fluid from your body. Filtering waste from the blood is essential for survival and protects every system in the body.
Creatinine, eGFR, uACR, and BUN are crucial markers for kidney patients. Your doctor will look at these to help determine how well your kidneys are working and removing waste.
Creatinine
Creatinine is a waste product made by your muscles from the breakdown of a compound called creatine. Because the kidneys are responsible for removing creatinine from your body, monitoring the amount of creatinine in your blood is a key way to check on the health of your kidneys.
There are several reasons why a creatinine level may be high – it could be a sign of worsening kidney function but it could also indicate dehydration, certain medications, infections, or possibly a diet very high in protein.
Your creatinine is used to calculate your estimated Glomerular Filtration Rate (eGFR), another key marker of your kidney’s function.
Estimated Glomerular Filtration Rate (eGFR)
One of the key markers for kidney function is your estimated Glomerular Filtration Rate (eGFR). It estimates how well your kidneys are filtering waste, toxins, and extra fluid from your body every minute. The eGFR is also useful to help detect kidney disease, track progression of the kidney disease, and also help guide treatment decisions.
The eGFR calculation is based on your blood creatinine level, age, sex, and sometimes race. It calculates how much blood is passing through the glomeruli (tiny filtering units in your kidneys) each minute.
The eGFR level is used to help determine how severe your kidney damage is from Stage 1 (mild) chronic kidney disease (CKD) to Stage 5 (end stage kidney failure).

Because your eGFR may fluctuate slightly based on your hydration status, medications you are taking (including over-the-counter medications), illness, and even your muscle mass, your healthcare provider will use the eGFR to help decide whether to start or stop medication. It is also used to help decide when you get referred to a nephrologist, and when to help prepare for dialysis or transplantation.
Urine Albumin-to-Creatinine Ratio (uACR)
The Urine Albumin-to-Creatinine Ratio (uACR) test is a tool to check for kidney damage. If you have diabetes or high blood pressure, you should have a uACR test regularly.
The presence of albumin (a protein found in the blood) in the urine (called albuminuria or proteinuria) is one of the earliest signs your kidneys are leaking protein, which is a sign of kidney disease.
The uACR test counts the amount of albumin in your urine compared to creatinine (a waste product, mentioned above). The result of your uACR is used together with your eGFR to determine the stage of kidney disease and the risk of your kidney disease progressing.
A high uACR is often linked with a higher risk of kidney failure, heart disease, and death.
Considerations if your uACR is elevated:
- Control blood sugar
- Manage blood pressure
- Reduce salt and protein intake
- Your healthcare provider may suggest taking kidney-protective medications like:
- » ACE inhibitors (a type of medication that » ARBs (another type of medication that lowers blood pressure), or
- » SGLT2 inhibitors (a type of medication used to treat type 2 diabetes)
Blood Urea Nitrogen (BUN)
The Blood Urea Nitrogen (BUN) is a common blood test that measures how much urea nitrogen is in your blood. When your body breaks down protein from food, it creates urea. Urea is a waste product. Urea travels through your blood to your kidneys and the kidneys will normally filter it out into your urine.
If you have kidney disease, urea builds up in your blood and causes a high BUN level. That is why the BUN value is another key marker when you have kidney disease as it helps assess how well your kidneys are removing waste products from your body.
BUN may also rise in the setting of dehydration, bleeding, high protein intake, or heart failure.
Along with your creatinine and your eGFR, your BUN is used to evaluate and track your CKD.
Electrolytes
Healthy kidneys are necessary for managing electrolytes. Electrolytes are minerals with an electric charge that are essential for bodily functions like nerve and muscle function, hydration, and maintaining pH balance. While the kidneys are filtering waste from your blood, they are also deciding how much of each electrolyte stays in the body and how much is removed from the body through the urine. Electrolytes that are important for kidney health include: potassium, sodium, calcium, phosphorus, and bicarbonate.
Potassium (K)
Potassium (K) is a mineral and electrolyte that is very important in regulating your heart rhythm and in supporting muscle and nerve function.
Your kidneys are responsible for filtering out excess potassium from your blood through the urine. If your kidneys cannot filter potassium, potassium will build up in the bloodstream. A high potassium level, also known as hyperkalemia, is life threatening because it may cause cardiac arrest. Learn more about potassium at www.areyouok.org and mark your calendar for National High Potassium Awareness Day (May 1st).
Sodium (Na)
Sodium (Na) is an electrolyte and is a mineral closely monitored to assess your fluid and blood pressure. When you have kidney disease, your kidneys may not be able to get rid of excess sodium. Excess sodium, also called hypernatremia, may lead to fluid retention, swelling (edema), high blood pressure (hypertension), and even congestive heart failure.
Calcium (Ca)
Calcium (Ca) is an electrolyte and a is a very important mineral in keeping bones and teeth strong and healthy. Calcium balance can be disrupted in kidney disease leading to serious complications which is why your calcium must be monitored closely in kidney disease. A high level of calcium in the blood is called hypercalcemia which can lead to various symptoms and complications such as bone weakening, kidney stones, and heart and brain dysfunction.
Calcium is the main mineral in bones (about 99% of calcium is stored there). Maintaining a balanced level of calcium in the blood is very important as it keeps our bones and teeth healthy but also helps with nerve function, muscle contractions, and blood clotting.
Calcium is closely regulated by other minerals and hormones, such as the parathyroid hormone, vitamin D, and calcitonin, a hormone produced by the thyroid gland that helps to lower blood calcium levels.
Hyperkalemia:
high potassium level in blood
Hypernatremia:
high sodium level in blood
Hypercalcemia:
high calcium level in blood
Bone and Mineral Balance
Kidneys play a key role in regulating calcium (see above) and other minerals, such as phosphorus, in your body.
Ensuring your bone-mineral levels are well-managed will aid in reducing long-term complications such as weak bones, calcium deposits in blood vessels, and heart disease.
Phosphorus (P)
Phosphorus (P) is another important electrolyte and mineral that is essential for bone formation, energy metabolism, and cell function. About 85% of phosphorus is stored in bones.
The kidneys are primarily responsible for helping maintain a balanced level by removing excess phosphorus. When the kidneys are not properly functioning, phosphorus can build up, causing hyperphosphatemia, and can bind with calcium pulling calcium out
of the bone - this causes those
calcium deposits (vascular calcification) and weak bones.
Learn more about phosphorus at
www.thehiddenpinkidneydisease.org and mark your calendar for National Phosphorus Awareness Day (April 5th).
Vitamin D
Vitamin D is a fat-soluble vitamin essential for bone health, immune function, and maintaining a balance between your calcium and phosphorus levels.
Vitamin D is inactive when first consumed and healthy kidneys activate that inactive vitamin D to an active form called calcitriol. This activation is a necessary step in helping your body absorb calcium from food.
When kidneys are not functioning properly, they cannot convert vitamin D into calcitriol so less calcium is absorbed from the intestines. Reduced calcium absorption may lead to low levels of calcium.
Because vitamin D is needed for calcium absorption, if the kidneys are not fully working, vitamin D will remain inactive, leading to: 1) low calcium 2) bone loss 3) overactive parathyroid glands (known as secondary hyperparathyroidism), and 4) higher risk of fractures.
Parathyroid Hormone (PTH)
The parathyroid glands are small endocrine glands (specialized organs that produce and secrete hormones) located behind your thyroid gland. The main function of the parathyroid glands is to regulate the level of calcium in your blood by producing a hormone called parathyroid hormone (PTH).
If the calcium level drops in your blood, the parathyroid glands will release PTH.

PTH works to increase calcium in the blood by:
- Releasing calcium from bones
- Increasing kidney reabsorption of calcium
- Activating vitamin D by increasing intestinal calcium absorption
- Promoting phosphate excretion
High levels of PTH is common in CKD. When PTH is high, it will pull calcium from bones and can cause bones to release calcium into the blood. Over time, this will weaken bones.
Secondary hyperparathyroidism is a condition in which the parathyroid glands produce too much PTH because of chronic low calcium levels caused by CKD. The effects of high PTH and low calcium include: renal osteodystrophy (a bone disease that occurs when CKD causes imbalances in minerals and hormones needed for healthy bones), calcification of blood vessels and tissues, muscle weakness, and joint pain. In some cases, a parathyroidectomy, or surgical removal of one or more parathyroid glands, may be considered to reduce these risks.
Hyperphosphatemia:
a condition when the phosphorus in the blood becomes higher than it should be
Hyperparathyroidism:
a condition where your body produces too much parathyroid hormone which can cause problems with your blood, bones, and kidneys
Renal osteodystrophy:
a bone disease that occurs when CKD causes imbalances in minerals and hormones needed for healthy bones
Parathyroidectomy:
surgical removal of one or more parathyroid glands
Anemia
Red blood cells (RBC) are the cells that travel throughout your body delivering oxygen to your organs, muscles and tissues. Anemia is when you do not have enough healthy red blood cells or hemoglobin to carry oxygen throughout the body. The kidneys are important in preventing anemia because they control the production of RBCs by making a very important hormone called erythropoietin.
Erythropoietin (EPO)
Erythropoietin (EPO) is a hormone produced by the kidneys and is released when the kidneys sense low oxygen levels in your blood. The hormone will tell your bone marrow to make red blood cells. When the kidneys are damaged, they may not produce enough EPO, so fewer RBCs are made, resulting in anemia.
Treatment for anemia associated with kidney disease typically includes:
- Iron supplements (oral or intravenous)
- Erythropoiesis-stimulating agents (ESA) which are injected under the skin (subcutaneously)
- Treating underlying causes like low vitamin B12 or chronic blood loss
Hemoglobin (Hb)
Hemoglobin (Hb) is a protein in red blood cells (RBCs) that transports oxygen from your lungs to the rest of your body. If you do not have enough hemoglobin, your organs, muscles and tissues will not get enough oxygen, leading to anemia.
If the hemoglobin drops too low, you may be at risk of heart failure because severe anemia makes your heart work harder.
Symptoms of anemia in CKD include:
- Fatigue
- Shortness of breath
- Weakness
- Pale skin
- Difficulty concentrating
- Reduced ability to exercise
- Chest pain or heart palpitations in severe anemia
Iron Studies (Ferritin, Transferrin Saturation)
Testing for iron helps your healthcare provider manage your anemia and provides them with a guide on what type of iron therapy may be needed. Iron is needed to create hemoglobin, the protein in red blood cells that carries oxygen from the lungs to the rest of the body.
Your healthcare provider may also screen your B12 and folate (vitamin B9) levels, as low levels of these may also lower hemoglobin.
Diabetes Screening
Screening for diabetes is very important because high blood sugar can damage the small blood vessels in the kidneys. Over time, this damage can lead to chronic kidney disease or even kidney failure.
Hemoglobin A1C (HbA1c)
Hemoglobin A1C (HbA1c) measures your average blood sugar level over the past 2-3 months and reflects how much glucose (sugar) has been attached to your red blood cells.
Hb A1c is an important tool to screen for diabetes. For persons with diabetes, it is also an important marker to evaluate how well the diabetes is being managed. Because diabetes is the leading cause of CKD, the HbA1c is especially important since uncontrolled blood sugar control contributes to worsening kidney disease by damaging the blood vessels in the kidneys. Over time this leads to protein in the urine, progression of the kidney disease, and even kidney failure.
The ideal HbA1c goal will depend on your stage of CKD, age and other health issues. Ensuring your Hgb A1c stays in a safe range will lower your risk of heart disease, nerve damage, and vision loss.
It is important to know that in later stages of CKD, HbA1c may be less reliable due to anemia, short red blood cell lifespan, or use of erythropoiesis-stimulating agents (ESA medications). In that case, your healthcare provider may also include a continuous glucose monitoring (CGM) device to assist with monitoring your blood sugar.
Urine Tests
Urine tests are an important tool when screening for kidney disease. Often, urine tests may show early signs of kidney disease – even before blood tests or before someone may have any physical symptoms of kidney disease.
Urinalysis
A urinalysis screens for protein in the urine (proteinuria), blood in the urine (hematuria), and other abnormalities, such as glucose (sugar) in the urine.
This test will also screen for white blood cells and nitrites – two signs that can indicate a urinary tract infection (UTI), which can worsen your kidney function if left untreated.
Albumin
Albumin is a protein made by the liver and works to keep fluid in your blood. If your body does not have enough albumin, fluid will leak into the tissues and cause swelling. Healthy kidneys help keep albumin in your blood where it belongs.
When kidneys are not properly functioning, albumin can leak into the urine, which is called albuminuria. High levels of albumin in urine is an early sign of kidney damage, which often appear before other symptoms. Low levels of albumin may suggest you are losing protein in your urine and may also indicate malnutrition.
The albumin level provides key information about your kidney function, nutritional status, and overall health and will be monitored to help track the progression of CKD.
Fluid and Acid-Base Balance
Kidneys are constantly monitoring and adjusting the amount of water and chemicals in your blood and tissues. Healthy kidneys are necessary to keep your body’s internal environment healthy and well-balanced.
Bicarbonate (HCO3-)
Bicarbonate (HCO3-) is an electrolyte and an alkaline substance (a substance that dissolves in water) that helps counteract excess acid in your blood. Healthy kidneys reabsorb bicarbonate and help to keep your blood pH (measure of the acidity or alkalinity of blood) stable.
In CKD, kidneys are not able to perform this function, leading to metabolic acidosis, or too much acid in the blood. Metabolic acidosis can worsen kidney damage.
Your bicarbonate level helps determine whether you will need to take oral sodium bicarbonate tablets or adjust your diet to help neutralize your blood.
Understand Your Lab Values!
Routine lab work is essential to managing your kidney disease and protecting your overall health. By learning and understanding your lab values, you will be an active participant in protecting your kidneys. As you keep track of lab values on your own, you can compare results from one report to another. Are they consistent? Is something higher or lower than previous labs? You can ask your doctor to explain any changes.
Benefits of understanding your lab values:
- Detect problems early
- Slow the progression of your kidney disease
- Avoid serious complications
- Improve quality of life and survival
- Know which lab values to ask your healthcare team about
- Participate in informed discussions with your healthcare team about what you can do to manage levels
Below is an example of a lab report you may have seen before, along with guidance on how to read and understand it.
Understanding your lab values is essential to managing your kidney disease. These values are monitored regularly and play a critical role in helping you and your healthcare provider:
- Track how well your kidneys are functioning
- Detect complications early
- Manage symptoms more effectively
- Guide treatment decisions to slow the progression of kidney disease
By learning what each lab value means, you can take a more active role in your care. This knowledge empowers you to ask informed questions, engage in meaningful conversations with your healthcare team, and ensure your questions and/or concerns are fully addressed. This brochure defines many of the tests and lab values that are important in managing kidney disease.
Kidney Function
Kidneys play a very important role in keeping your entire body functioning properly and have many responsibilities. One of those is to help filter waste and toxins from your blood and remove extra fluid from your body. Filtering waste from the blood is essential for survival and protects every system in the body.
Creatinine, eGFR, uACR, and BUN are crucial markers for kidney patients. Your doctor will look at these to help determine how well your kidneys are working and removing waste.
Creatinine
Creatinine is a waste product made by your muscles from the breakdown of a compound called creatine. Because the kidneys are responsible for removing creatinine from your body, monitoring the amount of creatinine in your blood is a key way to check on the health of your kidneys.
There are several reasons why a creatinine level may be high – it could be a sign of worsening kidney function but it could also indicate dehydration, certain medications, infections, or possibly a diet very high in protein.
Your creatinine is used to calculate your estimated Glomerular Filtration Rate (eGFR), another key marker of your kidney’s function.
Estimated Glomerular Filtration Rate (eGFR)
One of the key markers for kidney function is your estimated Glomerular Filtration Rate (eGFR). It estimates how well your kidneys are filtering waste, toxins, and extra fluid from your body every minute. The eGFR is also useful to help detect kidney disease, track progression of the kidney disease, and also help guide treatment decisions.
The eGFR calculation is based on your blood creatinine level, age, sex, and sometimes race. It calculates how much blood is passing through the glomeruli (tiny filtering units in your kidneys) each minute.
The eGFR level is used to help determine how severe your kidney damage is from Stage 1 (mild) chronic kidney disease (CKD) to Stage 5 (end stage kidney failure).

Because your eGFR may fluctuate slightly based on your hydration status, medications you are taking (including over-the-counter medications), illness, and even your muscle mass, your healthcare provider will use the eGFR to help decide whether to start or stop medication. It is also used to help decide when you get referred to a nephrologist, and when to help prepare for dialysis or transplantation.
Urine Albumin-to-Creatinine Ratio (uACR)
The Urine Albumin-to-Creatinine Ratio (uACR) test is a tool to check for kidney damage. If you have diabetes or high blood pressure, you should have a uACR test regularly.
The presence of albumin (a protein found in the blood) in the urine (called albuminuria or proteinuria) is one of the earliest signs your kidneys are leaking protein, which is a sign of kidney disease.
The uACR test counts the amount of albumin in your urine compared to creatinine (a waste product, mentioned above). The result of your uACR is used together with your eGFR to determine the stage of kidney disease and the risk of your kidney disease progressing.
A high uACR is often linked with a higher risk of kidney failure, heart disease, and death.
Considerations if your uACR is elevated:
- Control blood sugar
- Manage blood pressure
- Reduce salt and protein intake
- Your healthcare provider may suggest taking kidney-protective medications like:
- » ACE inhibitors (a type of medication that » ARBs (another type of medication that lowers blood pressure), or
- » SGLT2 inhibitors (a type of medication used to treat type 2 diabetes)
Blood Urea Nitrogen (BUN)
The Blood Urea Nitrogen (BUN) is a common blood test that measures how much urea nitrogen is in your blood. When your body breaks down protein from food, it creates urea. Urea is a waste product. Urea travels through your blood to your kidneys and the kidneys will normally filter it out into your urine.
If you have kidney disease, urea builds up in your blood and causes a high BUN level. That is why the BUN value is another key marker when you have kidney disease as it helps assess how well your kidneys are removing waste products from your body.
BUN may also rise in the setting of dehydration, bleeding, high protein intake, or heart failure.
Along with your creatinine and your eGFR, your BUN is used to evaluate and track your CKD.
Electrolytes
Healthy kidneys are necessary for managing electrolytes. Electrolytes are minerals with an electric charge that are essential for bodily functions like nerve and muscle function, hydration, and maintaining pH balance. While the kidneys are filtering waste from your blood, they are also deciding how much of each electrolyte stays in the body and how much is removed from the body through the urine. Electrolytes that are important for kidney health include: potassium, sodium, calcium, phosphorus, and bicarbonate.
Potassium (K)
Potassium (K) is a mineral and electrolyte that is very important in regulating your heart rhythm and in supporting muscle and nerve function.
Your kidneys are responsible for filtering out excess potassium from your blood through the urine. If your kidneys cannot filter potassium, potassium will build up in the bloodstream. A high potassium level, also known as hyperkalemia, is life threatening because it may cause cardiac arrest. Learn more about potassium at www.areyouok.org and mark your calendar for National High Potassium Awareness Day (May 1st).
Sodium (Na)
Sodium (Na) is an electrolyte and is a mineral closely monitored to assess your fluid and blood pressure. When you have kidney disease, your kidneys may not be able to get rid of excess sodium. Excess sodium, also called hypernatremia, may lead to fluid retention, swelling (edema), high blood pressure (hypertension), and even congestive heart failure.
Calcium (Ca)
Calcium (Ca) is an electrolyte and a is a very important mineral in keeping bones and teeth strong and healthy. Calcium balance can be disrupted in kidney disease leading to serious complications which is why your calcium must be monitored closely in kidney disease. A high level of calcium in the blood is called hypercalcemia which can lead to various symptoms and complications such as bone weakening, kidney stones, and heart and brain dysfunction.
Calcium is the main mineral in bones (about 99% of calcium is stored there). Maintaining a balanced level of calcium in the blood is very important as it keeps our bones and teeth healthy but also helps with nerve function, muscle contractions, and blood clotting.
Calcium is closely regulated by other minerals and hormones, such as the parathyroid hormone, vitamin D, and calcitonin, a hormone produced by the thyroid gland that helps to lower blood calcium levels.
Hyperkalemia:
high potassium level in blood
Hypernatremia:
high sodium level in blood
Hypercalcemia:
high calcium level in blood
Bone and Mineral Balance
Kidneys play a key role in regulating calcium (see above) and other minerals, such as phosphorus, in your body.
Ensuring your bone-mineral levels are well-managed will aid in reducing long-term complications such as weak bones, calcium deposits in blood vessels, and heart disease.
Phosphorus (P)
Phosphorus (P) is another important electrolyte and mineral that is essential for bone formation, energy metabolism, and cell function. About 85% of phosphorus is stored in bones.
The kidneys are primarily responsible for helping maintain a balanced level by removing excess phosphorus. When the kidneys are not properly functioning, phosphorus can build up, causing hyperphosphatemia, and can bind with calcium pulling calcium out
of the bone - this causes those
calcium deposits (vascular calcification) and weak bones.
Learn more about phosphorus at
www.thehiddenpinkidneydisease.org and mark your calendar for National Phosphorus Awareness Day (April 5th).
Vitamin D
Vitamin D is a fat-soluble vitamin essential for bone health, immune function, and maintaining a balance between your calcium and phosphorus levels.
Vitamin D is inactive when first consumed and healthy kidneys activate that inactive vitamin D to an active form called calcitriol. This activation is a necessary step in helping your body absorb calcium from food.
When kidneys are not functioning properly, they cannot convert vitamin D into calcitriol so less calcium is absorbed from the intestines. Reduced calcium absorption may lead to low levels of calcium.
Because vitamin D is needed for calcium absorption, if the kidneys are not fully working, vitamin D will remain inactive, leading to: 1) low calcium 2) bone loss 3) overactive parathyroid glands (known as secondary hyperparathyroidism), and 4) higher risk of fractures.
Parathyroid Hormone (PTH)
The parathyroid glands are small endocrine glands (specialized organs that produce and secrete hormones) located behind your thyroid gland. The main function of the parathyroid glands is to regulate the level of calcium in your blood by producing a hormone called parathyroid hormone (PTH).
If the calcium level drops in your blood, the parathyroid glands will release PTH.

PTH works to increase calcium in the blood by:
- Releasing calcium from bones
- Increasing kidney reabsorption of calcium
- Activating vitamin D by increasing intestinal calcium absorption
- Promoting phosphate excretion
High levels of PTH is common in CKD. When PTH is high, it will pull calcium from bones and can cause bones to release calcium into the blood. Over time, this will weaken bones.
Secondary hyperparathyroidism is a condition in which the parathyroid glands produce too much PTH because of chronic low calcium levels caused by CKD. The effects of high PTH and low calcium include: renal osteodystrophy (a bone disease that occurs when CKD causes imbalances in minerals and hormones needed for healthy bones), calcification of blood vessels and tissues, muscle weakness, and joint pain. In some cases, a parathyroidectomy, or surgical removal of one or more parathyroid glands, may be considered to reduce these risks.
Hyperphosphatemia:
a condition when the phosphorus in the blood becomes higher than it should be
Hyperparathyroidism:
a condition where your body produces too much parathyroid hormone which can cause problems with your blood, bones, and kidneys
Renal osteodystrophy:
a bone disease that occurs when CKD causes imbalances in minerals and hormones needed for healthy bones
Parathyroidectomy:
surgical removal of one or more parathyroid glands
Anemia
Red blood cells (RBC) are the cells that travel throughout your body delivering oxygen to your organs, muscles and tissues. Anemia is when you do not have enough healthy red blood cells or hemoglobin to carry oxygen throughout the body. The kidneys are important in preventing anemia because they control the production of RBCs by making a very important hormone called erythropoietin.
Erythropoietin (EPO)
Erythropoietin (EPO) is a hormone produced by the kidneys and is released when the kidneys sense low oxygen levels in your blood. The hormone will tell your bone marrow to make red blood cells. When the kidneys are damaged, they may not produce enough EPO, so fewer RBCs are made, resulting in anemia.
Treatment for anemia associated with kidney disease typically includes:
- Iron supplements (oral or intravenous)
- Erythropoiesis-stimulating agents (ESA) which are injected under the skin (subcutaneously)
- Treating underlying causes like low vitamin B12 or chronic blood loss
Hemoglobin (Hb)
Hemoglobin (Hb) is a protein in red blood cells (RBCs) that transports oxygen from your lungs to the rest of your body. If you do not have enough hemoglobin, your organs, muscles and tissues will not get enough oxygen, leading to anemia.
If the hemoglobin drops too low, you may be at risk of heart failure because severe anemia makes your heart work harder.
Symptoms of anemia in CKD include:
- Fatigue
- Shortness of breath
- Weakness
- Pale skin
- Difficulty concentrating
- Reduced ability to exercise
- Chest pain or heart palpitations in severe anemia
Iron Studies (Ferritin, Transferrin Saturation)
Testing for iron helps your healthcare provider manage your anemia and provides them with a guide on what type of iron therapy may be needed. Iron is needed to create hemoglobin, the protein in red blood cells that carries oxygen from the lungs to the rest of the body.
Your healthcare provider may also screen your B12 and folate (vitamin B9) levels, as low levels of these may also lower hemoglobin.
Diabetes Screening
Screening for diabetes is very important because high blood sugar can damage the small blood vessels in the kidneys. Over time, this damage can lead to chronic kidney disease or even kidney failure.
Hemoglobin A1C (HbA1c)
Hemoglobin A1C (HbA1c) measures your average blood sugar level over the past 2-3 months and reflects how much glucose (sugar) has been attached to your red blood cells.
Hb A1c is an important tool to screen for diabetes. For persons with diabetes, it is also an important marker to evaluate how well the diabetes is being managed. Because diabetes is the leading cause of CKD, the HbA1c is especially important since uncontrolled blood sugar control contributes to worsening kidney disease by damaging the blood vessels in the kidneys. Over time this leads to protein in the urine, progression of the kidney disease, and even kidney failure.
The ideal HbA1c goal will depend on your stage of CKD, age and other health issues. Ensuring your Hgb A1c stays in a safe range will lower your risk of heart disease, nerve damage, and vision loss.
It is important to know that in later stages of CKD, HbA1c may be less reliable due to anemia, short red blood cell lifespan, or use of erythropoiesis-stimulating agents (ESA medications). In that case, your healthcare provider may also include a continuous glucose monitoring (CGM) device to assist with monitoring your blood sugar.
Urine Tests
Urine tests are an important tool when screening for kidney disease. Often, urine tests may show early signs of kidney disease – even before blood tests or before someone may have any physical symptoms of kidney disease.
Urinalysis
A urinalysis screens for protein in the urine (proteinuria), blood in the urine (hematuria), and other abnormalities, such as glucose (sugar) in the urine.
This test will also screen for white blood cells and nitrites – two signs that can indicate a urinary tract infection (UTI), which can worsen your kidney function if left untreated.
Albumin
Albumin is a protein made by the liver and works to keep fluid in your blood. If your body does not have enough albumin, fluid will leak into the tissues and cause swelling. Healthy kidneys help keep albumin in your blood where it belongs.
When kidneys are not properly functioning, albumin can leak into the urine, which is called albuminuria. High levels of albumin in urine is an early sign of kidney damage, which often appear before other symptoms. Low levels of albumin may suggest you are losing protein in your urine and may also indicate malnutrition.
The albumin level provides key information about your kidney function, nutritional status, and overall health and will be monitored to help track the progression of CKD.
Fluid and Acid-Base Balance
Kidneys are constantly monitoring and adjusting the amount of water and chemicals in your blood and tissues. Healthy kidneys are necessary to keep your body’s internal environment healthy and well-balanced.
Bicarbonate (HCO3-)
Bicarbonate (HCO3-) is an electrolyte and an alkaline substance (a substance that dissolves in water) that helps counteract excess acid in your blood. Healthy kidneys reabsorb bicarbonate and help to keep your blood pH (measure of the acidity or alkalinity of blood) stable.
In CKD, kidneys are not able to perform this function, leading to metabolic acidosis, or too much acid in the blood. Metabolic acidosis can worsen kidney damage.
Your bicarbonate level helps determine whether you will need to take oral sodium bicarbonate tablets or adjust your diet to help neutralize your blood.
Understand Your Lab Values!
Routine lab work is essential to managing your kidney disease and protecting your overall health. By learning and understanding your lab values, you will be an active participant in protecting your kidneys. As you keep track of lab values on your own, you can compare results from one report to another. Are they consistent? Is something higher or lower than previous labs? You can ask your doctor to explain any changes.
Benefits of understanding your lab values:
- Detect problems early
- Slow the progression of your kidney disease
- Avoid serious complications
- Improve quality of life and survival
- Know which lab values to ask your healthcare team about
- Participate in informed discussions with your healthcare team about what you can do to manage levels
Below is an example of a lab report you may have seen before, along with guidance on how to read and understand it.
| Test | Normal Range | Additional Information |
| Creatinine | Female: 0.50–1.10 mg/dL Male: 0.70–1.30 mg/dL | |
| eGFR | 90-120 mL/min | Stage 1:90mL/min Stage 2: 60-89 mL/min Stage 3a:45-59 mL/min Stage 3b: 30-44 mL/min Stage 4: 15-29 mL/min Stage 5: 15 mL/min |
| BUN | 8-20 mg/dL | |
| Hemoglobin A1c | 4.0-5.6% | |
| UACR | Normal: 0-29 mg/g Moderately increased: 30-300 mg/g Severely increased: >300 mg/g | UACR >30mg/g is a marker for chronic kidney disease |
| Albumin | 3.5-5.5 g/dL | |
| Potassium | 3.5-5.0 mmol/L | |
| Sodium | 136-145 mmol/L | |
| Calcium | 8.6-10.2 mg/dL | |
| Phosphorus | 2.8-4.1 mg/dL | |
| Vitamin D, 25-hydroxy | 30-60 ng/dL | |
| PTH, Intact | 10-65 pg/mL | |
| Iron, serum Total Iron-binding Capacity (TIBC) Transferrin Saturation (TSAT) Ferritin< | 50–150 μg/dL 250-450 ug/dL 15-55% 15-150 ng/mL | Often an iron panel is checked. The iron panel includes several blood tests that collectively reveal how your body is storing and transporting iron. |
| Bicarbonate (CO2) | 23-30 mEq/L |
Disclaimer: Different laboratories may use slightly different reference ranges. Always review the range listed on your lab report and talk with your doctor about what your results mean for you.
Sources:
https://www.abim.org/Media/bfijryql/laboratory-reference-ranges.pdf
https://www.niddk.nih.gov/health-information/professionals/advanced-search/quick-reference-uacr-gfr
https://aakp.org/center-for-patient-research-and-education/hyperkalemia/
https://aakp.org/center-for-patient-research-and-education/high-phosphorus/


















